AI-Driven Radiomics for Precision Prostate Cancer Therapy
 3D Reconstruction of Human Olfactory System
3D Reconstruction of Human Olfactory System
AI-Driven Radiomics for Precision Prostate Cancer Therapy
Authors: Tsz Him Chan, Annette Haworth, Alan Wang, Mahyar Osanlouy et al.
Publication: EJNMMI Research (2023)
Code: Available on Request
Overview
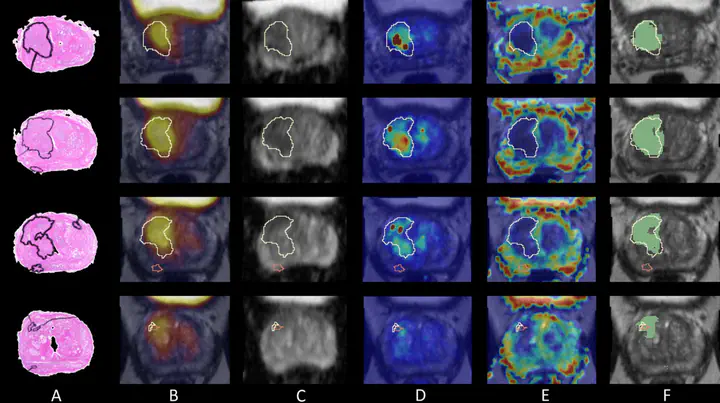
This pioneering study developed an AI-powered radiomics pipeline to optimize biologically targeted radiation therapy (BiRT) for prostate cancer. By integrating PSMA PET/CT with multiparametric MRI (mpMRI), we created voxel-level predictions of tumor location and grade through advanced image registration and machine learning techniques.
Key Innovations
- Multi-modal fusion: First study combining PSMA PET radiomics with DCE MRI perfusion parameters
- Voxel-wise prediction: Achieved 0.89 AUC for tumor detection using 3D radiomic features
- Grade differentiation: Developed two-stage RFC model separating high/low-grade disease (Accuracy: 0.67-0.99)
- HPC-optimized registration: Reduced spatial uncertainty to 3.3mm using deformable histology alignment
Computational Pipeline
1. Multi-modal Image Registration
- Data Integration: Co-registered PSMA PET/CT (5 scanners), mpMRI (2x Siemens 3T), and whole-mount histology
- Key Steps:
align_pet_ct() → rigid_registration(mpMRI) →
deformable_registration(ex_vivo_MRI) →
histology_annotation_propagation()
- Challenges Solved:
- Bladder filling artifacts in PET
- Partial volume effects in 3.27mm PET slices
- Non-linear prostate deformation post-resection
2. Radiomic Feature Engineering
| Modality | Features Extracted | Key Parameters |
|---|---|---|
| PSMA PET | 3D LoG, LBP, GLCM textures | SUVmax, metabolic tumor volume |
| DCE MRI | Ktrans, iAUGC60, TTP perfusion maps | Pharmacokinetic modeling |
| ADC Maps | NGTDM coarseness, percentile values | b=1200 s/mm² diffusion restriction |
Feature Selection:
- ANOVA filtering → Gini impurity ranking
- Final feature set: 50 most discriminative parameters
Machine Learning Architecture
Tumor Detection Model
- Two-stage RFC Framework:
- Location Detection: 842 sensitivity/804 specificity
- Grade Classification: Low vs High Grade (ISUP ≥3)
- Performance Comparison:
| Model | AUC | Sensitivity | Specificity |
|---|---|---|---|
| PET Alone | 0.865 | 0.781 | 0.799 |
| mpMRI Alone | 0.882 | 0.802 | 0.801 |
| Combined | 0.890 | 0.842 | 0.804 |

Receiver operating characteristics for different models
Key Radiomic Predictors
- PET: 3D LoG(σ=3mm) minimum
- ADC: NGTDM Coarseness
- DCE MRI: Ktrans 90th percentile
Clinical Implications
- Personalized Radiotherapy: Enables voxel-level dose painting based on metabolic/perfusion features
- Early Recurrence Prediction: High-grade lesions showed 2.8× higher PSMA uptake (p<0.01)
- Technical Impact:
- Solved partial volume effects in PET-guided planning
- Demonstrated perfusion > diffusion for grade prediction
- Open-source registration framework [3D Slicer Plugin]
Future Directions
- Multi-institutional validation across PET/MRI scanners
- DL Enhancement: Replace handcrafted features with 3D CNNs
- Real-time Adaptation: Integrate with MR-Linac systems
This project received funding from Prostate Cancer Foundation of Australia and Health Research Council of New Zealand.